GALAXY UM - PAYER UTILIZATION MANAGEMENT
Payer Utilization Management for Faster Decisions and Better Member Outcomes
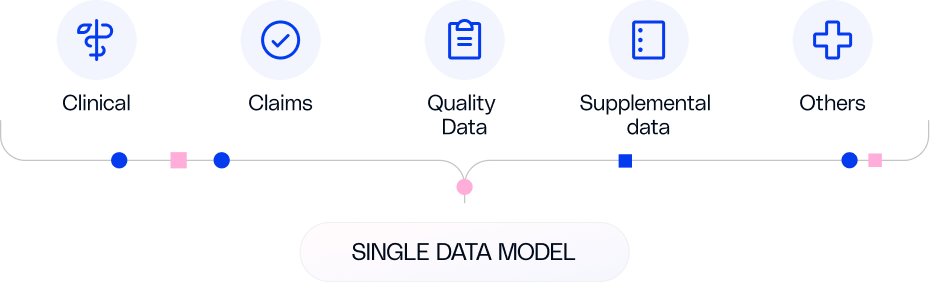
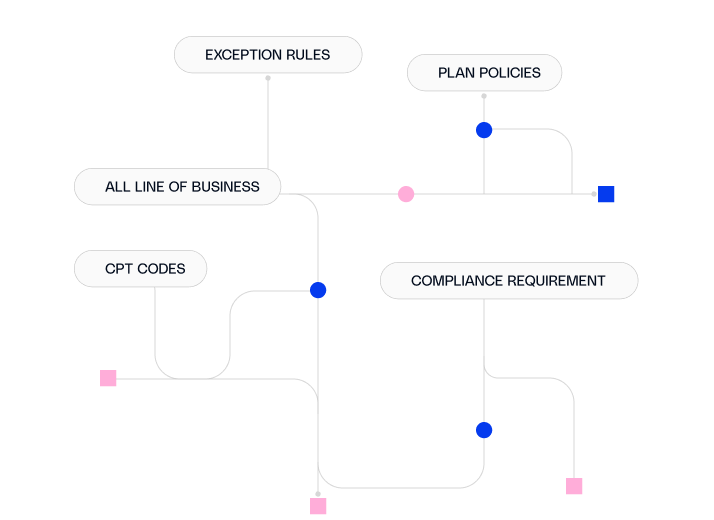
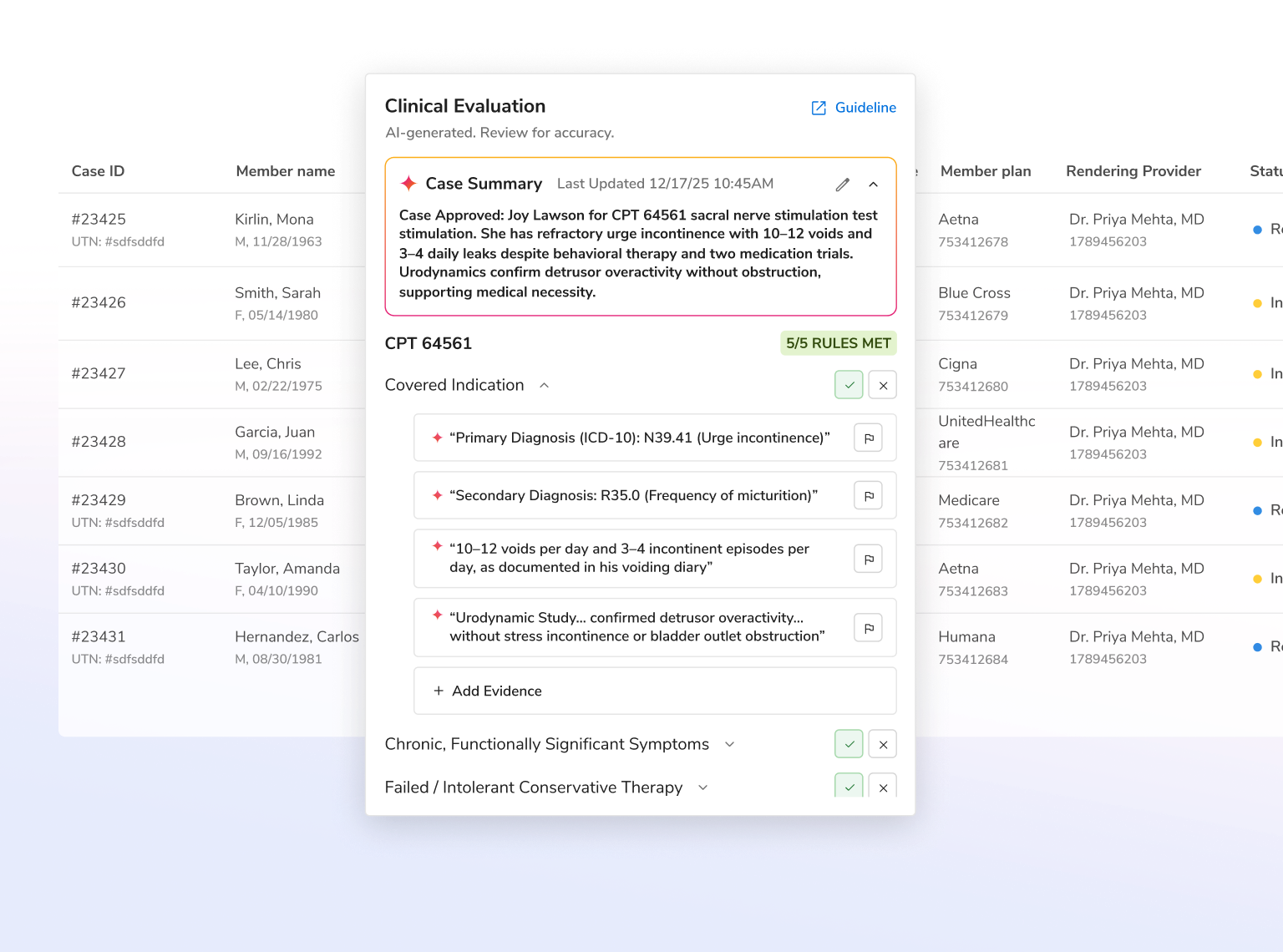
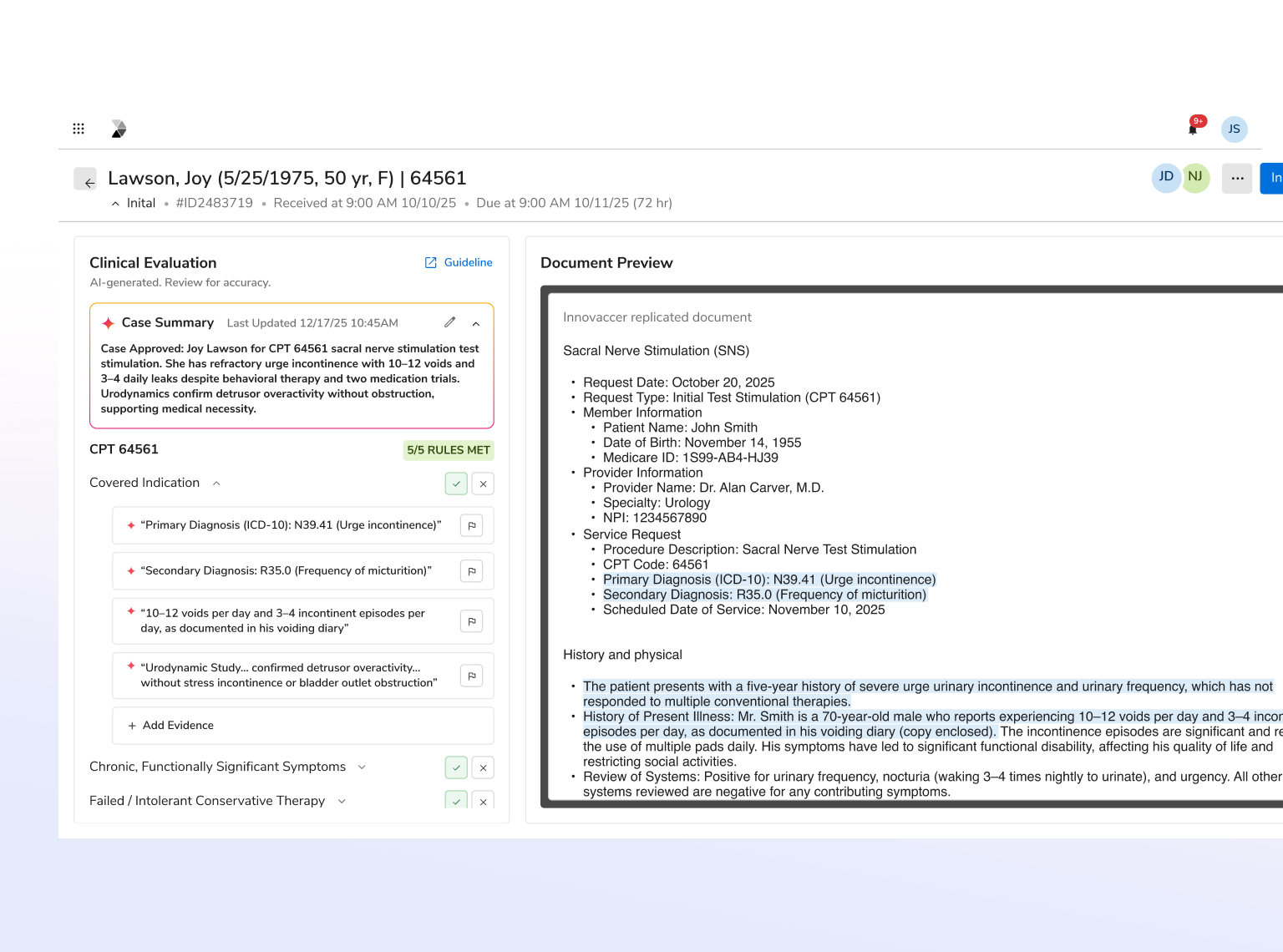
Agentic AI that automates end-to-end utilization management to reduce manual work, lower costs, and help members get the right care faster across all lines of business, guided by evidence-based criteria.


Innovaccer is trusted to deliver value at scale





.svg)









.png)
.png)
.png)