One Platform to Close up to 90% of HEDIS and Stars Gaps


Health plans depend on their HEDIS and Stars ratings. These scores impact access to quality bonus payments, with CMS distributing $12.7 billion to plans that achieve 4 stars or higher in 2025. For payers, strong performance across these measures means more revenue, a competitive edge, and better member retention.
What are HEDIS and Stars Measures?
Health plans' performance is measured through two primary frameworks: HEDIS and Star Ratings. While they are closely linked, they serve distinct purposes:
- HEDIS (Healthcare Effectiveness Data and Information Set) tracks over 90 specific measures across six domains, such as effectiveness of care, access/availability of care, experience of care, utilization and risk-adjusted utilization, health plan descriptive information, and Electronic Clinical Data System (ECDS) reporting to provide a granular look at clinical performance.
- Star Ratings is a performance-based system that evaluates plans on up to 43 measures, including clinical results, member experience, pharmacy performance, etc.
The bottom line is that high HEDIS scores are the essential building blocks that are required to achieve a meaningful Star Rating. Together, they provide a 360-degree view of how well a provider and health plan meet their members' needs.
The real challenge for payers isn't just understanding these metrics, but it’s the sheer scale of managing them. Monitoring 90+ measures across thousands of members requires a system that can:
- Identify performance gaps in real time.
- Coordinate immediate interventions.
- Accurately record outcomes for every single member.
Unfortunately, many plans are currently hitting a wall. Instead of a streamlined operation, they are relying on piecemeal systems: fragmented tools that tackle quality of care in silos. This lack of integration makes it nearly impossible to cut through the complexity, leaving payers struggling to move the needle on their ratings.
Why Traditional Gap Closure Methods Fail
The reason traditional methods fail isn’t a lack of clinical intent; it’s a data latency problem. Most plans operate in a retrospective vacuum, looking at data that is weeks or months old. By the time a gap is identified, the opportunity to influence the member's care has often already passed.
1. The "Silo" Tax
Quality improvement is currently a victim of fragmented architecture. When member outreach, clinical data, and pharmacy claims live on separate islands, the "left hand" never knows what the "right hand" is doing. For example, a quality team flags a diabetic member for an A1c test, unaware that the member visited a clinic yesterday. The data just hasn't been updated yet.
2. The "Chart-Chasing" Treadmill
Without a unified system, come HEDIS season, staff are forced into a manual marathon. They export spreadsheets, manually reconcile lists, and repeatedly badger provider offices for the same medical records for different measures. This "double work" doesn't just waste time; it leads to provider burnout and strained relationships with the very doctors the plan relies on for care.
3. Member Abrasion
The most significant casualty of fragmented systems is the member experience. When systems don't talk to each other, members experience:
- Redundant Outreach: Getting a call from a pharmacy, a care manager, and a robotic dialer all in the same week for the same issue.
- Coordination Gaps: Missing a preventive screening because the pharmacist filling their statin had no visibility into their overdue mammogram.
Traditional systems are reactive. They tell you what went wrong last quarter. But in a landscape where Star Ratings are increasingly tied to member experience and rapid response, a reactive strategy is a losing one. To close gaps effectively, plans must move away from piecemeal tools and toward a single source of truth.
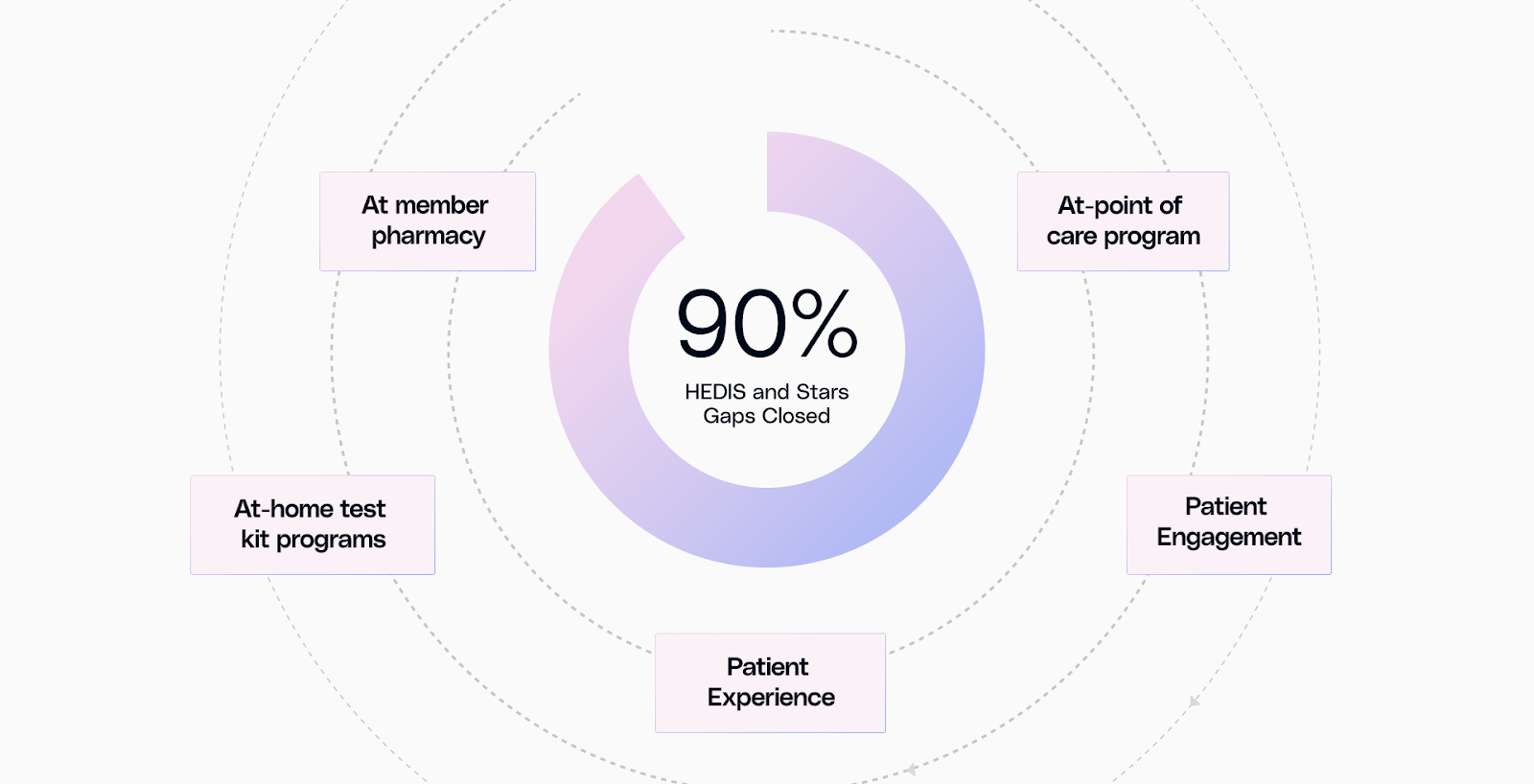
How Galaxy Unifies Gap Closure
Galaxy transforms quality management from a seasonal scramble into a continuous, automated engine. By unifying risk adjustment and quality control into a single interoperable platform, Galaxy eliminates the "data lag" that plagues traditional systems. It provides a single source of truth where AI-driven insights handle the heavy lifting, ensuring your team is audit-ready 365 days a year.
A Multi-Channel Approach to 5-Star Ratings
While traditional systems wait for claims to trickle in, Galaxy proactively closes gaps across three high-velocity channels, covering over 90% of HEDIS and Stars measures:
- AI-Driven Member Orchestration: Our AI doesn't just send reminders; it intelligently schedules appointments for critical screenings, like breast cancer and colorectal exams, while coordinating pharmacy interventions for diabetes and osteoporosis management.
- Integrated Provider Workflows: Galaxy bridges the gap between health plans and clinics by pushing real-time care opportunities directly into provider care management programs integrated with their quality management teams. Galaxy also highlights gap closure opportunities on point-of-care solutions during the member’s office visit.
- At-Home Assessment: Galaxy removes the friction of the doctor’s office by deploying at-home testing kits for A1c and colorectal cancer. By meeting members where they are, we see closure rates skyrocket.
- Real-Time Pharmacy Integration: This is where Galaxy truly shines. When a member visits the pharmacy for a routine refill, Galaxy instantly flags any missed preventive screenings. The pharmacist can provide an at-home test kit on the spot, the system records the intervention immediately, and the HEDIS report updates in real time.
Ending the "Chart-Chasing" Marathon
The most significant drain on a quality team’s time is manual record retrieval. Galaxy utilizes advanced AI for automated chart retrieval, coding, and abstraction. By synchronizing prospective, concurrent, and retrospective reviews into one workflow, Galaxy eliminates redundant "chases." The system identifies the evidence, validates the code, and closes the gap, reducing the administrative burden on your staff and providers alike.
Comprehensive Coverage Across Measures
Galaxy eliminates the traditional divide between clinical data and performance outcomes by providing comprehensive coverage for over 90% of all HEDIS and Stars measures. Rather than managing these frameworks in silos, the platform integrates core HEDIS metrics, such as childhood immunizations, prenatal care, and behavioral health, with critical Stars drivers like medication adherence, care transitions, and member experience. This dual-track visibility is delivered via real-time dashboards, allowing teams to monitor performance fluctuations across both frameworks simultaneously.
Beyond simple reporting, Galaxy utilizes predictive analytics to transform data into a strategic roadmap. The platform pinpoints members at the highest risk for hospitalization or critical care gaps, allowing plans to move from reactive "chart chasing" to proactive intervention. By prioritizing tasks based on their potential impact on overall ratings, Galaxy empowers quality teams to allocate their resources where they will most effectively drive clinical excellence and plan performance.
Measurable Results: From Compliance to Growth
Galaxy directly impacts your bottom line by providing the tools needed to elevate Star Ratings from 3 to 4, or 4 to 5 stars. These higher ratings unlock significant quality bonuses and drive member enrollment. By automating the identification of coding gaps for Medicare Advantage populations, the platform eliminates the manual bottlenecks that drain team resources.
Furthermore, Galaxy transforms audit prep into a continuous, year-round process. By maintaining CMS-compliant documentation and utilizing AI for automated chart retrieval, coding, and abstraction, the platform replaces the "last-minute scramble" with total audit readiness. This ensures high accuracy for RADV and OIG reviews while freeing your staff from the burden of manual labor.
Move Forward with Galaxy. Request a demo to see how Galaxy can improve your ratings while reducing the manual work that currently limits your teams.
Also read: How Health Plans Can Improve Star Ratings Through Multipoint Gap Closure.

.svg)


.png)



.png)



.avif)


.png)
.png)
.png)




.svg)
.svg)

.svg)

